Navigating Life's Detours
Finding the right path for a teen with special needs
I still do 27 years later

I was chatting with a coworker at AdventHealth and mentioned that today is my wedding anniversary. She asked how many years Paige Cousins and I have been married, and I responded, “27 years.” You could see the surprise in her eyes.
It doesn’t feel like that long. To me, it’s all a blur. The years seemed to move by much slower when I was younger. As I’ve moved into adulthood, I just want to hit the brakes and savor so many things, including the time I have with Paige.

But so many things seem to get in the way of our ability to just enjoy one another, and lately, I largely blame Covid, which seems to be the “worse” part of the “for better or worse” line in our wedding vows.
Covid has robbed us of the ability to do many of our favorite things, including dining out and having date nights. We’ve allowed fewer people into our home in an effort to protect J.P. from exposure to the dreaded virus.
Additionally, J.P. continues to grow, and with his adult body, he’s less mobile and requires more than one person to change his position and bathe, as well as more respiratory treatments and interventions to keep him comfortable.
Saying I feel trapped would be a misnomer, because we’ve been very lucky to still have our son with us. For those who have closely followed this blog over the years, you know we’re way beyond the life expectancy given to us for J.P.
But those ingredients you often hear about to have a successful marriage (i.e.: be romantic, prioritize one another, get away from the kids, schedule date nights) have been lost because of Covid and the necessities that come with caring for someone who’s reached adulthood despite significant medical needs.
So where do we go from here? We focus on our commitment to each other. We try to make time for one another at home. We take things day by day, and we focus on our blessings. We hold on to hope. Things won’t stay this way forever.

I often recall the many good times we’ve had. I’ve always believed that I was very lucky to have married into the Royalty family. Get-togethers before the pandemic always included great food and plenty of laughs. Holiday celebrations often lasted for several days. Vacations to see family in other parts of the country were fun-filled.
I recall so many great times spent with Paige. Movie nights, weekend getaways, trying new restaurants, watching our favorite TV shows at home. The memories of times-gone-by make me smile, but Covid has definitely been a bump in the road.
But as fast as the years are moving by lately, change is inevitable, and I’m forever grateful to have a life partner that’s equipped for whatever is thrown our way, and I’m thankful that she treasures the commitment she made to me 27 years ago.
Happy anniversary, Paige!

Friday Fun: An update from Karina

Hi there, It’s Karina.
Several years ago, I spoke to you about my job as J.P.’s service dog. I was practically a puppy at the time, and a fresh graduate from Canine Companions for Independence.
“A dog is the only thing on earth that loves you more than he loves himself.”
Josh Billings
It’s been a great career. I’ve become a member of the family, and enjoy cuddling up with J.P. during the day, and I even get to snuggle with Paige at night.
I’m 7 years old now, which is the equivalent of 47 human years. I’m holding up pretty well. I think I’m still pretty well behaved, and Jeff has kept a close eye on my weight, so treats are very limited.
I do get two peanut butter-flavored Pill Pockets each evening. That’s because I have to take two milk thistle capsules because of some poor liver numbers. My veterinarian is keeping a close eye on that.
I still know most of my Canine Companion commands. I mostly hear, “Hurry,” which means to potty, “OK,” which means I can eat, “Jump,” to get on the couch, and “Off,” to get back on the floor. Each night, I’m told to “Kennel,” which means to get in my kennel in J.P.’s room and go to bed.
Before my last recertification exam, I showed Jeff and Paige that I still know several other commands, which aren’t used as often.
- Tug: Dog will pull a strap with its mouth
- Push: Dog closes a door or drawer
- Get: Dog retrieves an item with its mouth
- Give: Dog releases grip on item in its mouth while person’s hand is on the item

I love my job. I’m just not a big fan when J.P. is admitted to the hospital, and I spend a lot of time home alone. I watch over J.P. and say prayers that he stays healthy, so I can remain by his side as his best furry friend.
Now, can we talk about that cat? He can be a pain.
Sleepless nights

We’re going through something, and it hasn’t been much fun.
One of the things I’ve always treasured about our life with J.P. is that he’s been a pretty good sleeper. I’ve heard many stories from parents of special needs kids who have terrible sleepers.
“Sleep is the Swiss army knife of health. When sleep is deficient, there is sickness and disease. And when sleep is abundant, there is vitality and health.”
Matthew Walker
They’re either up all night, up half the night, up every few hours. Whatever they’re going through, I feel for them. It’s not fun, and it doesn’t set things up to have a very good day afterward. When it continues night after night, everyone becomes edgy and short, you can make bad choices and say things you don’t mean.
One thing I’ve learned in my 49 years of life is that I’m not a night person. I might have been in my teen years, but that is not the case anymore. I’m ready for bed at 9 p.m., and I wake up before 6 a.m. and feel like I’m ready to tackle the day. I might even decide to go for a jog and watch the sun rise. It’s a good time, really.

J.P. has recently decided to either be fussy at bedtime or to whine in the middle of the night. We still have a monitor in his room, so we get to hear it all. When this happens on occasion, it’s fine. I can get up, give him some Advil and go back to bed. But when it happens night after night, we’ve learned you can’t keep giving Advil because it can mess with his liver.
We have some other medicines we can also use, but there are repercussions with those, too. They can make him sound junky the next day, and then we have to put him on his belly and try to keep his oxygen level up.
I’m not sure what’s going on. He could be in the middle of a period of cluster headaches. His doctor has said it may just be teen angst, but I can tell you I’m not a fan.
I want my boy to get back to his good sleeping regimen, so we can all wake up feeling refreshed again. I’m sure he would like that, too.
The J.P. Story: Hospital holidays

Dad’s note: In honor of J.P.’s 12th birthday, I began writing “The J.P. Story,” which looks back at our journey through birth and into childhood. I hope you’ve enjoyed it. The 13th chapter continues to examine the challenges we’ve faced with cluster headaches and hospitalizations. To start at the beginning of the story, click here.
We’ve learned a lot about J.P. over the years, and one thing he’s done pretty consistently is to end up in the hospital around the holidays. He has also spent several birthdays there. I theorize that it could be that he likes to return to his place of birth on his birthday, but he has also been there on Paige’s and my birthdays. That’s a bit harder to understand.
It was beginning to look like we may be spending Thanksgiving and Christmas in the hospital in 2018. Unexplained pain and recurrent vomiting had sent us to the hospital in October and again in early November. We were discharged after a five-day stay and returned to the emergency room that night.
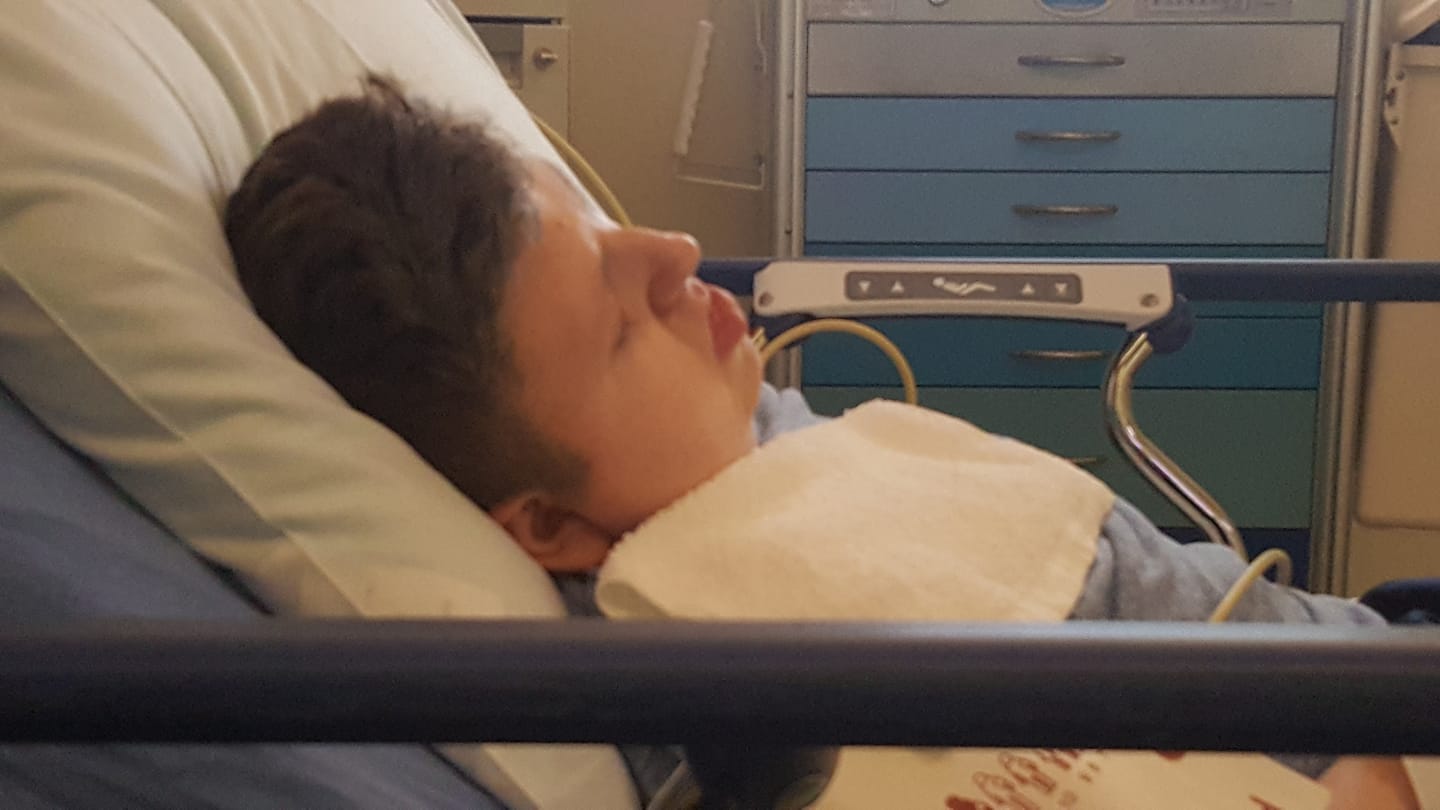
We knew the drill at this point, and so did many of the staff in the emergency department. However, we had a doctor who hadn’t worked with J.P. before, and despite our pleas and those of some of his consulting doctors, this doctor felt J.P. didn’t require admission to the PICU. We were placed in the Pediatric Medical/Surgical Unit. The hospital’s computers were also down, so that added another degree of complexity to everything.
I took the overnight shift with J.P., and we ended up in our room about 2 a.m. I spoke to a medical student who would be caring for him and was told that the chief resident would be coming by soon. I let the nurse and medical student know that we needed to get IV fluids started as soon as possible because of his diabetes insipidus. (J.P. can become dehydrated quickly when he’s not eating and frequently vomiting.)
I was exhausted at this point. J.P. had fallen asleep with the anti-nausea medications, and I settled in on the parent bed and hoped to hear from the chief resident soon. However, I closed my eyes and next thing I knew it was about 6 a.m. J.P. was still asleep, and there were no IV fluids running. I called the nurse and was told there was a delay in getting the appropriate fluids because of the computer downtime. I reiterated that J.P. has diabetes insipidus and can’t be off fluids for an extended period.
I contacted J.P.’s endocrinologist, who quickly called the attending doctor and was able to get the IV fluids ordered stat. J.P. had another vomiting episode and dropped his oxygen level to the point where he was rapid-responsed back to PICU, which was where we wanted him placed initially.
At this point, my stress level was through the roof, and I was beyond the point of exhaustion and couldn’t take much more. The news we would get in the coming days led to us to try to move his feeding tube to his intestines, but subsequent vomiting dislodged the tube.
My sister was closely following things from Missouri and had heard enough. She came to our rescue at the end of November, and we learned a few days later that J.P. was ready to go home. After all that had happened, there was an element of fear to going home. I felt I might lose my mind if he were to vomit again, but at least three of us would be ready in a worst-case scenario.
I tried to think positively. This is the Christmas season, right? The best gift ever would be to be able to put this behind us. We could get some decorations out for the holidays. Maybe my sister could help us decorate our tree. That would be a lot of fun, and I was definitely ready for something fun. But then it happened. It seemed to come from nowhere. J.P. was vomiting again, and my heart just sank.
Just like before, the respiratory issues followed the vomiting, and we were back on the phone with the 911 operators. The fire engine and ambulance were soon at our house, and before we knew it, we were back where we least wanted to be: the emergency room. The hopes that this nightmare was over were dashed. Christmas was again on hold, and our hearts were broken.
Two days later I wrote a post to Facebook that summed up my feelings.
“These have been among the roughest days as the dad of a child with special needs. The back and forth to the hospital, the vomiting, the difficulty to find a diagnosis, and the lack of treatment options have taken a toll. Throw in a few unexpected twists, and it’s been exhausting both mentally and physically for Paige Royalty Cousins and myself. I apologize for not updating sooner, but here’s what I can share: J.P. isn’t a kid anymore. He’s 16 years old, and it’s more difficult for his malformed brain to regulate everything with a bigger body. This means the motility of his digestive system is slowing, and it’s not likely to get any better in the future. We’re planning to try a formula that’s easier to digest and feed him at a bit of a higher rate for fewer hours each day to give his gut more time to rest. If that doesn’t work we may attempt placing another GJ-tube, but he’s not a great candidate for that. Long story short, none of our options are a permanent fix, things are likely to get worse over time, and we need to think long and hard about where to draw the line with interventions. It sucks, and there’s probably more vomit in our future. I will say on a brighter note that our core team is doing all they can to work together with the intensivists on the plan. The past 48 hours has seen all of J.P.’s docs racking their brains to figure this out, and I greatly appreciate their efforts, as well as my sister, Catherine Cousins Brandt, for extending her stay to help Paige and I through everything.”
Posted to Facebook on Dec. 5, 2018
This hospital stay left us with little patience. The doctors gave us little hope that they would be able to solve the problem. Some questioned why there was so much vomiting at home and repeatedly questioned us on whether we were part of the problem. It was decided that wasn’t the case once they talked to the medical professionals that know our family best.
We’ve repeatedly been told that kids with special needs usually have more problems in adult bodies. There is more that the brain, heart and lungs must manage, and they’re already working quite hard before all the growth is completed. That’s something I try to keep tucked away in the deep recesses of my mind and try not to think too much about because I can’t do anything about it.
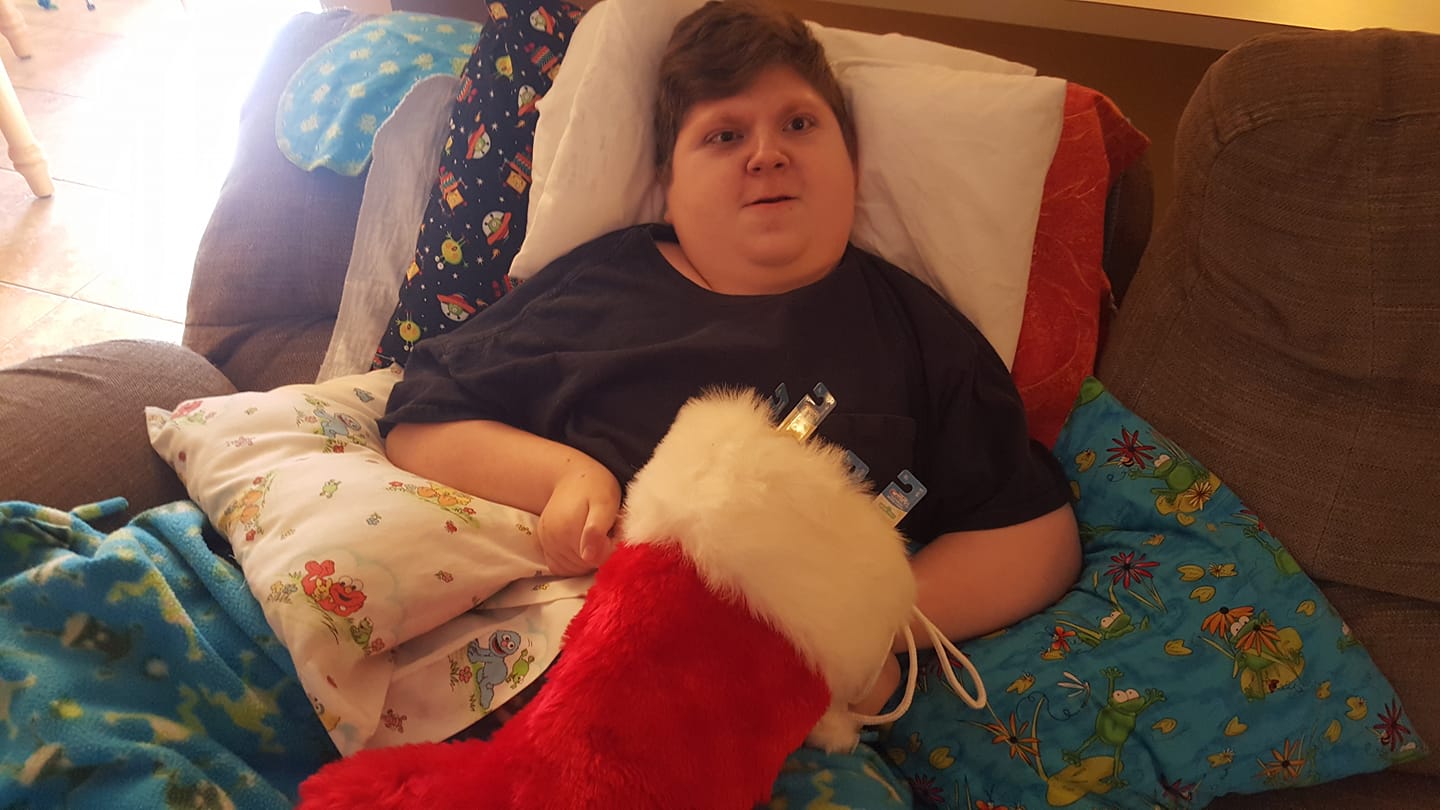
We did make it home in time for Christmas, and while it was more low key than some, it was also special to really spend time simply appreciating the fact that we were home with close family and thankful that we didn’t have to add Christmas to the list of holidays where we’ve been inpatient.
The J.P. Story: Problems with pain

Dad’s note: In honor of J.P.’s 12th birthday, I began writing “The J.P. Story,” which looks back at our journey through birth and into childhood. I hope you’ve enjoyed it. The 12th chapter looks at the challenges we’ve faced with cluster headaches and hospitalizations. To start at the beginning of the story, click here.
Having a teenager who can’t talk comes with many challenges, but one of the most frustrating is when they can’t tell you what hurts when they’re sick. With many different diagnoses to manage, it can be difficult to know what doctor to contact when issues arise, and many of the symptoms of all of J.P.’s illnesses can be pain and nausea.
J.P. began vomiting in October, and we weren’t sure if it was because of cluster headaches, gastrointestinal issues or a shunt malfunction. I’m not talking about the kind of vomiting when you feel better after it happens. This was vomiting that wouldn’t cease, and eventually led to respiratory distress and a 911 call.

Again, J.P. can’t tell us what he’s feeling, so we rushed him to the hospital by ambulance. He was admitted, and we began our search for answers. He continued to vomit in the emergency room, and he was close to being intubated because of the low oxygen level.
We were sent to the PICU. Multiple tests were ordered, and consults were placed for gastroenterology, endocrinology, neurology and neurosurgery to rule out a shunt malfunction. There were so many questions: Does he feel sick to his stomach, or is the nausea more because he’s light-headed or dizzy? Is he having a cluster headache? No answers seemed to come easy, but a decision was made to check his shunt, which ended up being OK.
We spent several days working to get feeds established, and as we were preparing for discharge, we learned his sodium level was too high. At the same time, his IV infiltrated, which would be key to bringing down his sodium level. Things improved from there, and we were discharged two days later.
We were home for about two weeks, before a follow-up appointment with J.P.’s endocrinologist that ended with breathing problems and another ambulance ride to the hospital. During this admission, there was a noticeable change in the way things were communicated with us regarding the long-term implications to our son’s life.
It felt like the providers were ready to just write everything off to J.P.’s underlying diagnoses, but Paige and I weren’t ready to throw in the towel. Some of the doctors who know him best weren’t around, but the others who were did offer support and ideas to try to get J.P. eating again.
We were desperate to find hope. Hearing some of the common things people would say didn’t help. Things like, “God won’t give you more than you can handle,” just irritated me. I read a Facebook post from Lysa TerKeurst that states it wasn’t even something God said.
God does say He won’t allow us to be tempted beyond what we can bear and that He always provides a way out. (1 Corinthians 10:13) But that’s not the same as God not giving us more than we can handle … The world is filled with people who are dealt more than they can handle. And, surprisingly, so is the Bible.
The Apostle Paul wrote: “We do not want you to be uninformed, brothers and sisters, about the troubles we experienced in the province of Asia. We were under great pressure, far beyond our ability to endure, so that we despaired of life itself. Indeed, we felt we had received the sentence of death. But this happened that we might not rely on ourselves but on God, who raises the dead” (2 Corinthians 1:8-9, NIV).
What incredible hope for our hearts. God doesn’t expect us to handle this. He wants us to hand this over to Him.
Lysa TerKeurst

During these vomiting episodes, J.P. would begin to sound very junky. With the impact that was having on his oxygen level, we figured out that placing him on his stomach would quickly improve his oxygen saturation level. On several occasions it has allowed us to avoid intubation. Some of our nurses and respiratory therapists were amazed at the difference it would make. One of our doctors even put in an order that we flip him three times a day.
AdventHealth has a STAR Program for children with special needs. They’ve invested in having special toys and activities available to make the inpatient experience more pleasant. We started to bring some of those toys into the room for J.P. while he was on his belly, and he loved looking at the lights (pictured, above).
J.P. was able to go home two days later. We were ready for a break, but after just eight hours we were in the Children’s Emergency Center again with the same symptoms and few answers. We were desperate for help.
The J.P. Story: Uncharted waters

Dad’s note: In honor of J.P.’s 12th birthday, I began writing “The J.P. Story,” which looks back at our journey through birth and into childhood. I hope you’ve enjoyed it. The 11th chapter looks at the changes having a teenager has brought to our lives. To start at the beginning of the story, click here.

When J.P. turned 13 years old, it was a milestone and reason to celebrate. While J.P. was considered by most to be a miracle baby, his medical challenges had the doctors warning us that he would likely never become a teenager.
We were entering uncharted waters with our boy, and we weren’t alone. Studies have shown about 750,000 children with special needs in the United States transition from pediatric to adult care every year, and while J.P. is still a few years away from making the move, health care systems across the country are struggling to find care for these patients as they reach adulthood.
“Finding adult primary and specialty care providers for youth with chronic conditions has been a challenge for pediatricians, youth and families,” said Wake Forest Baptist Health Dr. Paul J. Sagerman, who co-chaired a study on the topic.
“Travelers are always discoverers, especially those who travel by air. There are no signposts in the sky to show a man has passed that way before. There are no channels marked. The flier breaks each second into new uncharted seas.”
Anne Morrow Lindbergh

While the transition to adult care is always on my mind, there was a more immediate concern to deal with: J.P. was growing, and it was becoming more difficult for one person to care for him alone.
Our Home and Community-Based Services waiver through Medicaid allowed us to add a lift system in J.P.’s bedroom and our family room in 2015, but as helpful as the lift is, there are still times every day when he needs to maneuvered on the couch, especially for diaper changes. We’ve also been lucky enough to have nurses from Aveanna Healthcare in our home, some of whom have become more like family. The extra hands can be a big help as he’s grown.
When it comes to school, J.P. remains enrolled in Seminole County Public Schools and his pediatrician believes the Hospital-Homebound Program is best for him. That means his teachers and therapists come to our home each week for one-on-one education. He is currently enrolled in high school.

Despite the school changes, his educational team has remained largely intact, and he seems to enjoy the time with his teachers. He still loves books, and gets pretty decent grades. He can remain in school until he turns 22, and then we’ll need to determine some next steps for him.
There are two programs that I’m keeping my eye on. an adult program through the Conductive Education Center of Orlando, and Community Art Connection at Northland Church. Those are decisions for a different day (or year).
For now, it’s important to continue to enjoy J.P. for the teenager he has become. His smile remains precious, his personality engaging and his health stable. He’s come a long way for a kid who was never supposed to make it to high school.
Continue to Chapter 12: Problems with pain
World of change


It was British Prime Minister Benjamin Disraeli who first said that change is inevitable, and I’ve seen plenty of it over the past three years. When I last posted to this blog, I was leaving my life in TV news to reinvent myself as a family-centered care consultant at Florida Hospital for Children in Orlando.
There were no guarantees. This was a new position that was created as a test. It was a leap of faith on my part that the many people who got to know me through numerous hospital stays and time spent on the Family Advisory Council would see the value to having a parent around who could help to improve the experience of our patients and families.
As with anything new, there’s paperwork and approvals needed. Florida Hospital is a huge entity, so it took some time to get the necessary paperwork completed, and I was a stay-at-home dad for about four months.
But the timing couldn’t have been more perfect. My father-in-law and mother-in-law both had to be hospitalized during my time at home. My wife needed to help care for them during their recovery, and while she focused on getting them better, I was able to focus on J.P., and see all it takes to keep our boy on track.

I believe it also helped me get ready for my new role at Florida Hospital for Children. Spending long hours at the TV station isn’t conducive to being a hands-on dad, but that’s exactly what I needed to know to be empathetic to parents dealing with their sick kids, as well as doctors, nurses and other care providers.
My future wasn’t going to revolve around broadcasting information anymore. The most important thing I would be doing is listening, understanding and comforting — and helping our clinicians to do the same thing. Having had so much experience with J.P. at the hospital helps me understand the feelings and occasional frustrations that can be felt along the way.
J.P. has really grown over the past three years. Getting the ceiling lift in 2015 was a convenience at the time, but it’s definitely a necessity now. Having a nurse every day to help Paige with diaper changes and medicines is also much more important.
He’s in high school now, and we’re dealing with brutal cluster headaches that can bring him to tears, and we ended up with a very long and messy hospital stay at the end of 2018 because of unrelenting vomiting that will be the subject of a future post.
That hospital admission was the first where I was challenged to balance my dad and hospital employee roles. It wasn’t the perfect hospital admission, but it was great to see that despite some issues, everyone viewed it as a learning experience, and we vowed to work together to improve things in the future.
I’m happy to say that my role at what is now AdventHealth for Children has grown. I’m a full-time employee now, and I also oversee GetWellNetwork for our campus. I was honored to receive the Partner In Care award last year, and I recently traveled to Washington, D.C., for system manager training at GetWellNetwork headquarters. I was also featured in FHTV News with my former WESH coworker Mike O’Lenick.
I’m a member of several hospital councils, including our Shared Leadership Quality and Practice Council. I’m also on several committees and continue to assist with the Family Advisory Council, which is comprised of our NICU, pediatric, teen and e-councils.

So why has it been three years without a post to the blog? Well, I lost access to it. The blog was under my Hearst email address, and somehow I forgot my password. It couldn’t be reset, because I no longer had my Hearst email. There were numerous phone calls and emails to WordPress that went nowhere, but I persevered, and this week was able to get a helpful individual who understood the importance of what I’m doing here.
It’s really taken on new meaning with my hospital position. I’m hearing the stories of so many parents, and I have the ability to share my experiences to help them find their way when change seems so inevitable.
Thanks for the memory

“Thanks for the memory
Of rainy afternoons, swingy Harlem tunes
Motor trips and burning lips and burning toast and prunes.
How lovely it was.”
I’ve seen a lot of people come and go in my years at WESH-TV, and I always thought of the tune Bob Hope made famous on someone’s last day.
I’ve heard many people who come to WESH from other stations say that it is unique when it comes to the camaraderie among those who work here.
For a sense of how strong that is, I called WESH home for more than 27 years, and there are plenty of people still working at the station who’ve been there for more than 30 years.
WESH is family, and I guess that’s why I never thought I would be walking out the doors of the station to work somewhere else.
But I’ve learned how much life experiences can change someone, and the things I’ve been through make my career move exciting.
As much as I’ve changed, I’ve also learned so much from my time at WESH. I entered the newsroom as an intern at the age of 18. I was there when the station moved their Daytona Beach and Orlando studios. I was different. Television was different.
I was playing miniature golf on a date on Aug. 2, 1990, when the first bombs fell on Baghdad at the start of the Persian Gulf War. I rushed to the station to help out. In the weeks afterward, I remember the networks breaking into programming to watch Patriot missiles take out Scud missiles launched from Iraq.
I was producing the 11 p.m. news on the night of Feb. 22, 1998, when a series of tornadoes hit Central Florida and killed 42 people. I was in the control room throughout the night, and our first live shot was done by our sports anchorman, Buddy Pittman, who jumped in a live truck and went to Winter Garden after hearing that an apartment complex was seriously damaged.
I remember sitting at my desk watching the coverage of the first plane hitting the World Trade Center on Sept. 11, 2001, and meteorologist Mike O’Lenick and I both wondered if it was really a passenger jet. I heard Claire Metz scream, “Oh my God,” when the second plane hit and everything seemed much more sinister.
It was on my birthday, Feb. 1, 2003, when I was waiting for Columbia to land before I could leave to go to my party with family. Columbia never made it to the runway at Kennedy Space Center, and I missed my own celebration to make sure the coverage was handled on WESH.com.
They were crazy times, and I learned early in my career that news can happen anytime, regardless of what plans you may have or personal situations that are ongoing.
It can wear you down, and I won’t miss the crazy schedules that sometimes go along with a career in the news industry.

My wife once said that if she were ever going to write a book, it would be titled, “How NASA Ruined My Marriage.” I spent many days at Kennedy Space Center covering shuttle launches for the website, and if the launch was scrubbed, it just meant going back out for the next attempt, and the one after that.
But part of me also wonders how I’ll feel when the next big story breaks, and I’m not in the newsroom learning all the latest details as they happen. That need to know doesn’t just go away instantly.
At least I can rest easy knowing that all my friends at WESH will keep digging and bringing me those details I crave while I watch on TV or online from the comfort of my living room, with my wife and child by my side.
This news veteran is trading in his keyboard to help parents face more personal challenges when their kids are hospitalized, and they’re looking for answers they won’t find on TV.
“Awfully glad I met you
Cheerio and toodle-oo
Thank you
Thank you so much.”
J.P.’s hospital stay: 1 month later

It’s been one month since J.P. arrived at Florida Hospital for Children by ambulance. It was the week before Thanksgiving, and we prayed we would make it home in time to celebrate Turkey Day with our family.
I can’t believe we’re now wondering if we’ll be home for Christmas, and I’m beginning to believe the answer is probably no.
We’ve never spent Christmas in the hospital. When J.P. was much younger, we paid a visit to his neurologist’s office for a VNS setting change on Dec. 25, but this would be the first time inpatient.
We haven’t yet broken our record for longest stay in the hospital — which is 35 days — but we’re getting awfully close.
I recently wrote about some of the lessons I’ve learned from this hospital stay, but I’m also beginning to understand the emotional and physical toll these stays have on parents of chronically ill children.
The most apparent thing I’ve noticed after 30 days in the hospital is a difficulty to answer simple questions from a nurse or doctor. They ask questions like, “How long has his central line been in place?” or “When was his second shunt surgery?” I have no idea.
I can say something like, “The central line was placed during his second surgery,” But I can’t tell them immediately when that was. The days have all blurred together.
I haven’t had problems trying to determine a course of action after certain medical events have taken place. J.P. is vomiting again, so I know we need to stop feeds and return to IV fluids. Give his tummy a break, and restart feeds slowly.
I even know that we need to give him a dose of Zofran when we restart the feeds. If we still have issues, we should investigate using Reglan or consider possibly returning to a GJ feeding tube instead of a G tube.
But I’m weary, and I know my wife is weary. We’re trying to hold it together, but we’re short with one another and don’t always agree on what to do next.
I’m eating more junk food than I should, and I’ve gained weight. I’m not running much, and I don’t have the energy I’m used to having. I am trying to climb the stairs at the hospital instead of taking the elevator.
I’m sad. I’ve heard some things from doctors that scare me to the core. Some doctors I can dismiss and say they haven’t been on J.P.’s case long and don’t know him like we do. But when the doctors who do know J.P. make an observation about his quality of life or longevity, It just hits me hard, and I sometimes feel like an emotional wreck.
It’s all happening during a time when I’m used to celebrating the holiday season, and that’s been stolen this year by the Grinch, it seems. Seriously.
Our house is a clear indicator that Christmas didn’t come this year. No lights. No trees. No decorations.
It’s a consequence you face when you have a medically complex child, and there’s nothing I can do about it. At this point, I’m not sure if it’s even going to get better in the near future or if it could get worse.
Following my heart

From a very young age, I always knew what I wanted to do when I grew up. I was fascinated with television and spent my childhood dreaming about working at the TV station.
Saying “the TV station” above is not a mistake, because there was one station to which I was drawn, WESH-TV.
I watched the station religiously and was fascinated with the many facets of local TV news. It wasn’t just the glamour factor. I was intrigued by everything about it — the live trucks, cameras, sets, control room, editing, videotape, master control — every bit of it.
In junior high, I learned even more about it by becoming a media aide and was on the fast track to a place in the television production class in high school. I was even more excited to learn I could be a part of the school’s weekly newscast.
Instead of dreading that I had to go to school each day, I began to love it. I learned all about those facets of TV that amazed me. We operated cameras, edited stories, wrote scripts, created graphics, learned how to operate a switcher — I was in heaven.
I decided I was going to break into the business at WESH-TV and called just before I graduated and asked if I could be an intern. I was told they didn’t have a program like that, and I said I would be happy to be their first intern. It worked.
I spent 18 months as an intern and was hired as a production assistant in 1989. I eventually became a producer and moved to the growing field of online journalism when WESH launched NewsChannel2000.com in 2000.
But my world took a detour two years later when my wife and I had our first child. Our son, J.P., was born with a form of cerebral palsy, holoprosencephaly, and numerous other disorders, like hydrocephalus, diabetes insidious, epilepsy, spastic quadriplegia — the list goes on and on.
Some things happened in the days before J.P. was born that changed me and my outlook on life.
Minutes after learning that our precious boy would be born with significant disabilities, doctors were telling my wife and I that she was putting her life at risk by carrying J.P. and needed to be admitted to the hospital to terminate the pregnancy. They said we needed to make the decision immediately.
I have always been the type to listen to what a doctor says, but this was a decision that just couldn’t be made that fast. Somehow, Paige and I were able to get out of the hospital and learned that there was really no additional risk to Paige. They considered the additional risk to be due to the fact that our boy would have no quality of life, so there was no reason to put her through the risks of the pregnancy.
We changed our doctor and decided to deliver at Florida Hospital in Orlando, where the staff supported our decision and surrounded us with the hope and belief that God had a plan for J.P. That plan is still going on 14 years later.
In that time, I’ve learned a great deal about the importance of care that is patient- and family-centered. I’ve learned how that type of care improves patient safety. I joined Florida Hospital for Children’s Family Advisory Council and served as chairman of it for three years. I’ve also served as a member of the Nursing Governance Council and currently serve on the Patient Safety and Quality Committee.
When the Florida Legislature was considering deep cuts to Medicaid funding, I traveled to Tallahassee with a team of doctors and nurses to share the importance of protecting the program for our kids. I delivered a speech at the State Capitol and talked to legislators. The hospital also paid for me and two other family advisors to attend a conference in Tampa by the Institute for Patient- and Family-Centered Care.
My world has changed since I began my career in TV news 27 years ago. There were the jubilant moments when my son was born and he was in such good health that he didn’t even have to go to NICU, and there have been times when I wondered if J.P. would survive to see the next day. I’ve seen parents broken by the loss of a child, and doctors who needed to discuss a care plan for a baby whose parents never came to the hospital or even returned a phone call.
My experiences have led me to a decision to leave WESH-TV at the end of December. I tell people it’s the only place I’ve worked other than McDonald’s.
But the battles my family has conquered since J.P.’s birth have taught me plenty, and I need to use the skills I’ve learned in the journalism field — great communication — to help other families who are facing situations that seem insurmountable.
So even when J.P. isn’t a patient at Florida Hospital for Children, I plan to be there to help the many families in need make sure their care is family-centered and that they’re playing a role in the care plan.
For now, I’ll be doing that on a volunteer basis, but I’m confident that the position will grow into something permanent, and the hospital’s commitment to family-centered care makes taking the chance worthwhile.
I’m so excited about this opportunity to make a difference for families and children who need help to get through tough times like my family has faced.
I consider myself twice as lucky that I get to again create something that doesn’t currently exist just like I created that internship at an incredible TV station so many years ago.